Childhood Soft Tissue Sarcoma (PDQ®)–Patient Version
What is childhood soft tissue sarcoma?
Childhood soft tissue sarcoma is cancer that forms in muscle, fat, fibrous tissue, blood vessels, or other supporting tissue of the body.
Soft tissues of the body connect, support, and surround other body parts and organs. The soft tissues include:
- fat
- bone
- cartilage
- fibrous tissue
- muscles
- nerves
- tendons (bands of tissue that connect muscles to bones)
- synovial tissues (tissues around joints)
- blood vessels
- lymph vessels
Soft tissue sarcoma may occur anywhere in the body. In children, the tumors form most often in the arms, legs, chest, or abdomen.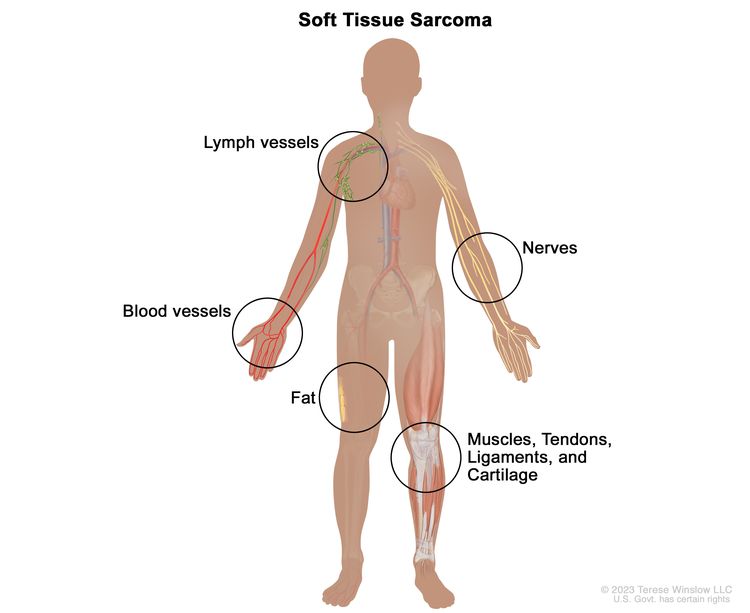
Soft tissue sarcoma occurs in children and adults. Soft tissue sarcoma in children may respond differently to treatment and may have a better prognosis than soft tissue sarcoma in adults. Learn more about soft tissue sarcoma in adults at Soft Tissue Sarcoma Treatment.
Types of soft tissue sarcoma
There are many types of soft tissue sarcoma. They are grouped based on the type of soft tissue cell where they first formed.
This summary is about the following types of soft tissue sarcoma:
Blood vessel tumors
Blood vessel tumors include the following types:
- Epithelioid hemangioendothelioma. Epithelioid hemangioendothelioma can occur in children but is most common in adults between 30 and 50 years. It may occur in the liver, lung, bone, skin, or soft tissue. Epithelioid hemangioendothelioma may be fast growing or slow growing. In about a third of patients with a tumor in the soft tissue, the tumor spreads to other parts of the body very quickly. Learn more at Childhood Vascular Tumors.
- Angiosarcoma. Angiosarcoma is a fast-growing cancer that forms in the blood vessels or lymph vessels in any part of the body, usually in the soft tissue. Most angiosarcomas are in the skin or in the soft tissue near the skin. Those in deeper soft tissue can form in the liver, spleen, and lung. This cancer is very rare in children. Children sometimes have more than one tumor in the skin, liver, or both. Rarely, infantile hemangioma may become angiosarcoma. Learn more at Childhood Vascular Tumors.
Bone tumors
Extraskeletal osteosarcoma. This type of bone and cartilage cancer is very rare in children and adolescents. It is likely to come back after treatment and may spread to the lungs. Osteosarcoma occurs more often in bone.
Cartilage tumors
Extraskeletal mesenchymal chondrosarcoma. This type of cartilage cancer often affects young adults and occurs in the head and neck. It is usually high grade (likely to grow quickly) and may spread to other parts of the body. It may also come back many years after treatment.
Fat tissue tumors
Liposarcoma. This is a cancer of the fat cells. Liposarcoma usually forms in the fat layer just under the skin. In children and adolescents, liposarcoma is often low grade (likely to grow and spread slowly). Liposarcoma may spread to the lungs and rarely to the lymph nodes. There are several different types of liposarcoma, including:
- Myxoid liposarcoma. Learn about Myxoid/Round Cell Liposarcoma.
- Myxoid pleomorphic liposarcoma. This is a rare cancer that most often forms in the middle of the chest in children, adolescents, and young adults. This cancer is high grade and can grow quickly and spread to other areas in the body.
- Pleomorphic liposarcoma. This is usually a high-grade cancer that is less likely to respond well to treatment. Pleomorphic liposarcoma often forms in older adults.
Fibrous connective tissue tumors
Fibrous connective tissue tumors have several subtypes, including:
- Desmoid-type fibromatosis. Learn about Desmoid Tumor.
- Dermatofibrosarcoma protuberans. This is a cancer of the deep layers of the skin that most often forms in the trunk, arms, or legs. Dermatofibrosarcoma protuberans usually does not spread to the lymph nodes or other parts of the body.
Some cancers have cells with a certain genetic change called a translocation (part of one chromosome switches places with part of another chromosome). In dermatofibrosarcoma protuberans, an abnormal gene is formed when the COL1A1 gene switches places with part of the PDGFRB gene. To diagnose dermatofibrosarcoma protuberans, the cancer cells are checked for this genetic change.
- Inflammatory myofibroblastic tumor. This rare tumor can occur in the soft tissue or organs in children and young adults. Learn about Inflammatory Myofibroblastic Tumor (IMT).
- Fibrosarcoma. There are two types of fibrosarcoma in children and adolescents:
- Infantile fibrosarcoma (also called congenital fibrosarcoma). This type of fibrosarcoma usually occurs in children 1 year and younger and may be seen in a prenatal ultrasound exam. This cancer is fast growing and is often large at diagnosis. It rarely spreads to distant parts of the body.
Some cancers have cells with a certain genetic change called a translocation (part of one chromosome switches places with part of another chromosome). In infantile fibrosarcoma, an abnormal gene is formed when the ETV6 gene on chromosome 12 switches places with the NTRK3 gene on another chromosome. To diagnose infantile fibrosarcoma, the cancer cells are checked for this genetic change. A similar tumor has been seen in older children, but it does not have the translocation that is often seen in younger children. Other abnormal genes involved in infantile fibrosarcoma are BRAF, ALK, RAF1, GOLGA4, LRRFIP2, and CLIP1.
- Adult-type fibrosarcoma. This is the same fibrosarcoma found in adults. The cells of this cancer do not have the genetic change found in infantile fibrosarcoma. Learn more about soft tissue sarcoma in adults at Soft Tissue Sarcoma Treatment.
- Infantile fibrosarcoma (also called congenital fibrosarcoma). This type of fibrosarcoma usually occurs in children 1 year and younger and may be seen in a prenatal ultrasound exam. This cancer is fast growing and is often large at diagnosis. It rarely spreads to distant parts of the body.
- Myxofibrosarcoma. This is a rare fibrous tissue cancer that occurs less often in children than in adults.
- Low-grade fibromyxoid sarcoma. This is a slow-growing cancer that forms deep in the arms or legs and mostly affects young and middle-aged adults. The cancer may come back many years after treatment and spread to the lungs and the lining of the chest wall. Lifelong follow-up is needed.
- Sclerosing epithelioid fibrosarcoma. Learn about Sclerosing Epithelioid Fibrosarcoma.
Pericytic (perivascular) tumors
Pericytic tumors form in cells that wrap around blood vessels. There are different types of pericytic tumors, including:
- Myopericytoma. Infantile hemangiopericytoma is a type of myopericytoma. Children younger than 1 year at the time of diagnosis may have a better prognosis. In children older than 1 year, infantile hemangiopericytoma is more likely to spread to other parts of the body, including the lymph nodes and lungs.
- Infantile myofibromatosis. Infantile myofibromatosis is another type of myopericytoma. It often occurs in the skin of children younger than 2 years. Learn about Infantile Myofibromatosis.
Peripheral nerve sheath tumor
The nerve sheath is made up of protective layers of myelin that cover nerve cells that are not part of the brain or spinal cord. Learn about Malignant Peripheral Nerve Sheath Tumor.
Skeletal muscle tumors
Skeletal muscle is attached to bones and helps the body move.
- Rhabdomyosarcoma. Rhabdomyosarcoma is the most common childhood soft tissue sarcoma in children 14 years and younger. Learn more about Childhood Rhabdomyosarcoma Treatment.
- Ectomesenchymoma. This is a fast-growing tumor that occurs mainly in children. Ectomesenchymoma may form in the eye socket, abdomen, arms, or legs.
Smooth muscle tumors
Smooth muscle lines the inside of blood vessels and hollow internal organs such as the stomach, intestines, bladder, and uterus. Learn about Leiomyosarcoma.
So-called fibrohistiocytic tumors
- Plexiform fibrohistiocytic tumor. This is a rare tumor that usually affects children and young adults. The tumor usually starts as a painless growth on or just under the skin on the arm, hand, or wrist. It may rarely spread to nearby lymph nodes or to the lungs.
Tumors of unknown cell origin
Tumors of unknown cell origin (the type of cell the tumor first formed in is not known) have many subtypes, including:
- Myxoma. Myxoma is a tumor that can occur in the heart or skin. This tumor is frequently seen in children with Carney complex. Carney complex is a rare condition marked by spots on the skin, and tumors in the heart, endocrine glands, skin, and nerves. Carney complex may be linked to gene changes in the PRKAR1A gene.
- Synovial sarcoma. Synovial sarcoma is a common type of soft tissue sarcoma in children and adolescents. Learn about Synovial Sarcoma.
- Epithelioid sarcoma. This is a rare sarcoma that usually starts deep in soft tissue as a slow growing, firm lump and may spread to the lymph nodes. If cancer formed in the arms, legs, or buttocks, a sentinel lymph node biopsy may be done to check for cancer in the lymph nodes. Epithelioid sarcoma is linked to a change in a tumor suppressor gene called SMARCB1. This type of gene makes a protein that helps control cell growth.
- Alveolar soft part sarcoma. This tumor occurs in adolescents and young adults. Learn about Alveolar Soft Part Sarcoma (ASPS).
- Clear cell sarcoma. This cancer occurs in older children and young adults. Learn about Clear Cell Sarcoma.
- Extraskeletal myxoid chondrosarcoma. This type of soft tissue sarcoma may occur in children and adolescents. Over time, it tends to spread to other parts of the body, including the lymph nodes and lungs. The tumor may come back many years after treatment.
- Extraskeletal Ewing sarcoma. This cancer most often occurs in the bone but can form in the soft tissue. Learn more about Ewing Sarcoma Treatment.
- Desmoplastic small round cell tumor. This tumor usually forms in the abdomen. Learn about Desmoplastic Small Round Cell Tumors (DSRCT).
- Extrarenal (extracranial) rhabdoid tumor. Rhabdoid tumor most often occurs in the kidney or the brain, but can form in the soft tissues. Learn about Extra-Cranial Malignant Rhabdoid Tumor (MRT).
- Perivascular epithelioid cell tumors (PEComas). Benign PEComas may occur in children with an inherited condition called tuberous sclerosis. They occur in the stomach, intestines, lungs, and genitourinary organs. PEComas grow slowly, and most are not likely to spread.
- Undifferentiated or unclassified sarcoma. These tumors usually occur in the bones or muscles that help the body move.
- Undifferentiated pleomorphic sarcoma (malignant fibrous histiocytoma). This type of soft tissue tumor may form in parts of the body where people have received radiation therapy in the past, or as a second cancer in children with retinoblastoma. The cancer usually forms in the arms or legs and may spread to other parts of the body. Learn more about Osteosarcoma Treatment.
- Intracranial mesenchymal tumor. This type of malignant tumor forms in the brain of children, adolescents, and young adults.
Causes and risk factors for childhood soft tissue sarcoma
Childhood soft tissue sarcoma is caused by certain changes to the way soft tissue cells function, especially how they grow and divide into new cells. Often, the exact cause of these changes is unknown. Learn more about how cancer develops at What Is Cancer?
A risk factor is anything that increases the chance of getting a disease. Not every child with one or more of these risk factors will develop a soft tissue sarcoma. And it will develop in some children who don't have a known risk factor.
The risk of soft tissue sarcoma may be increased if your child has one of the following inherited disorders:
Another risk factor is past treatment with radiation therapy.
Talk with your child's doctor if you think your child may be at risk.
Symptoms of childhood soft tissue sarcoma
Soft tissue sarcoma may appear as a painless lump under the skin, often on an arm, a leg, the chest, or the abdomen. There may be no other symptoms at first. As the sarcoma gets bigger and presses on nearby organs, nerves, muscles, or blood vessels, it may cause symptoms, such as pain or weakness. Fever, weight loss, night sweats, and low or high blood sugar levels are rare symptoms.
Other conditions may cause the same symptoms. Check with your child's doctor if your child has any of these problems.
Tests to diagnose childhood soft tissue sarcoma
If your child has symptoms that suggest a soft tissue sarcoma, the doctor will need to find out if these are due to cancer or another problem. The doctor will ask when the symptoms started and how often your child has been having them. They will also ask about your child's personal and family medical history and do a physical exam. Depending on these results, they may recommend tests to find out if your child has a soft tissue sarcoma, and if so, its extent (stage).
The following tests may be used to diagnose soft tissue sarcomas. The results of these tests will also help you and your child's doctor plan treatment.
X-ray
X-ray is a type of radiation that can go through the body and make pictures of areas inside the body.
Magnetic resonance imaging (MRI)
MRI uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas in the body, such as the chest, abdomen, arms, or legs. This procedure is also called nuclear magnetic resonance imaging (NMRI).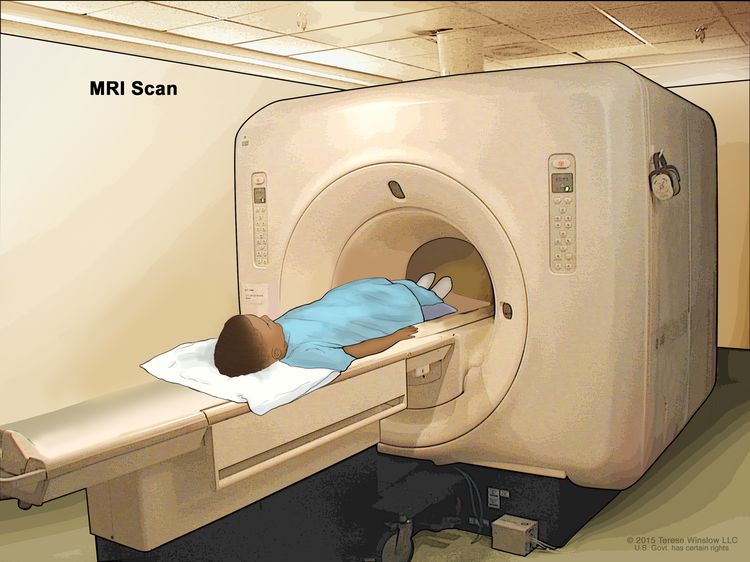
CT scan
CT scan (CAT scan) uses a computer linked to an x-ray machine to make a series of detailed pictures of areas inside the body, such as the chest or abdomen. The pictures are taken from different angles and are used to create 3-D views of tissues and organs. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography. Learn more about Computed Tomography (CT) Scans and Cancer.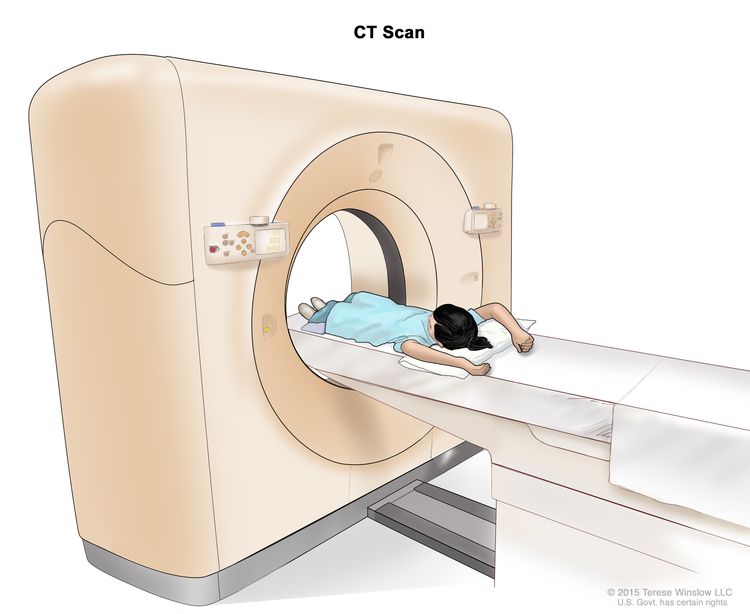
Ultrasound
Ultrasound uses high-energy sound waves (ultrasound) that bounce off internal tissues or organs and make echoes. The echoes form a picture of body tissues called a sonogram.
Biopsy
Biopsy is the removal of a sample of cells or tissue from the tumor so that a pathologist can view it under a microscope to check for cancer. The type of biopsy depends, in part, on the size of the mass and whether it is close to the surface of the skin or deeper in the tissue. The following types of biopsies may be used to check for soft tissue sarcoma:
- Core needle biopsy removes tissue using a wide needle. Multiple tissue samples are taken. This procedure may be guided using ultrasound, CT scan, or MRI.
- Incisional biopsy removes part of a lump or a sample of tissue.
- Excisional biopsy removes an entire lump or area of tissue that doesn't look normal. A pathologist views the tissue under a microscope to look for cancer cells. An excisional biopsy may be used to completely remove smaller tumors that are near the surface of the skin. This type of biopsy is rarely used because cancer cells may remain after the biopsy. If cancer cells remain, the cancer may come back, or it may spread to other parts of the body.
An MRI of the tumor is done before the excisional biopsy. This is done to make a picture of where the original tumor formed and may be used to guide future surgery or radiation therapy.
If possible, it is important to have the same surgeon perform the biopsy and the surgery to remove the tumor. The placement of needles or incisions for the biopsy can affect whether the tumor can be completely removed during a future surgery.
To plan the best treatment, the sample of tissue removed during the biopsy must be large enough to find out the type of soft tissue sarcoma and do other laboratory tests. Tissue samples will be taken from the primary tumor, lymph nodes, and other areas that may have cancer cells. A pathologist views the tissue under a microscope to look for cancer cells and to find out the type and grade of the tumor. The grade of a tumor depends on how abnormal the cancer cells look under a microscope and how quickly the cells are dividing. High-grade and mid-grade tumors usually grow and spread more quickly than low-grade tumors.
One or more of the following laboratory tests may be done to study the tissue samples:
- Light and electron microscopy checks cells in a sample of tissue under regular and high-powered microscopes to look for certain changes.
- Immunocytochemistry uses antibodies to check for certain antigens (markers) in a sample of a patient's cells or tissues. The antibodies are usually linked to an enzyme or fluorescent dye. After the antibodies bind to a specific antigen in the tissue sample, the enzyme or dye is activated, and the antigen can then be seen under a microscope. This type of test may be used to tell one type of soft tissue sarcoma from another type.
- Reverse transcription–polymerase chain reaction (RT-PCR) is a laboratory method used to make many copies of a specific genetic sequence for analysis. It may be used to look for certain changes in a gene or chromosome or for activation of certain genes, which may help diagnose a disease, such as cancer.
- Cytogenetic analysis checks the chromosomes of cells in a sample of tumor tissue for broken, missing, rearranged, or extra chromosomes. Changes in certain chromosomes may be a sign of cancer. Cytogenetic analysis is used to help diagnose cancer, plan treatment, or find out how well treatment is working. Fluorescence in situ hybridization (FISH) is a type of cytogenetic analysis.
- Molecular test checks for certain genes, proteins, or other molecules in a sample of tissue, blood, or bone marrow. Molecular tests also check for certain changes in a gene or chromosome that may cause or affect the chance of developing soft tissue sarcoma. A molecular test will often help determine the type of soft tissue sarcoma.
The Molecular Characterization Initiative offers free molecular testing to children, adolescents, and young adults with certain types of newly diagnosed cancer. The program is offered through NCI's Childhood Cancer Data Initiative. To learn more, visit About the Molecular Characterization Initiative.
The following tests may be used to find out if cancer has spread:
Sentinel lymph node biopsy
Sentinel lymph node biopsy removes the sentinel lymph node during surgery. The sentinel lymph node is the first lymph node in a group of lymph nodes to receive lymphatic drainage from the primary tumor. It is therefore the first lymph node the cancer is likely to spread to from the primary tumor. To identify the sentinel lymph node, a radioactive substance, blue dye, or both is injected near the tumor. The substance or dye flows through the lymph ducts to the lymph nodes. The first lymph node to receive the substance or dye is removed. A pathologist views the tissue under a microscope to look for cancer cells. If cancer cells are found, more lymph nodes will be removed through a separate incision (cut). This is called a lymph node dissection. Sometimes, a sentinel lymph node is found in more than one group of nodes. This procedure is used for epithelioid sarcoma.
PET-CT scan
PET-CT scan combines the pictures from a positron emission tomography (PET) scan and a computed tomography (CT) scan. The PET and CT scans are done at the same time on the same machine. The combined scans make more detailed pictures than either test would make by itself.
- For the PET scan, a small amount of radioactive sugar (also called radioactive glucose) is injected into a vein. The PET scanner rotates around the body and makes pictures of where sugar is being used in the body. Cancer cells show up brighter in the picture because they are more active and take up more sugar than normal cells do.
- For the CT scan (CAT scan), a series of detailed x-ray pictures are taken from different angles and are used to create 3-D views of tissues and organs. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography. Learn more about Computed Tomography (CT) Scans and Cancer.
Getting a second opinion
You may want to get a second opinion to confirm your child's cancer diagnosis and treatment plan. If you seek a second opinion, you will need to get medical test results and reports from the first doctor to share with the second doctor. The second doctor will review the genetic test results, pathology report, slides, and scans. This doctor may agree with the first doctor, suggest changes or another approach, or provide more information about your child's tumor.
To learn more about choosing a doctor and getting a second opinion, visit Finding Cancer Care. You can contact NCI's Cancer Information Service via chat, email, or phone (both in English and Spanish) for help finding a doctor or hospital that can provide a second opinion. For questions you might want to ask at your appointments, visit Questions to Ask Your Doctor about Cancer.
Types of treatment for childhood soft tissue sarcoma
Who treats children with soft tissue sarcoma?
A pediatric oncologist, a doctor who specializes in treating children with cancer, oversees treatment for soft tissue sarcoma. The pediatric oncologist works with other health care providers who are experts in treating children with soft tissue sarcoma and who specialize in certain areas of medicine. These may include a pediatric surgeon with special training in the removal of soft tissue sarcomas. Other specialists may include:
There are different types of treatment for children and adolescents with soft tissue sarcoma. You and your child's cancer care team will work together to decide treatment. Often, the treatments depend on the type of soft tissue sarcoma. Many other factors will be considered, such as your child's overall health and whether the cancer is newly diagnosed or has come back.
Your child's treatment plan will include information about the cancer, the goals of treatment, treatment options, and the possible side effects. It will be helpful to talk with your child's cancer care team before treatment begins about what to expect. For help every step of the way, visit our booklet, Children with Cancer: A Guide for Parents.
Types of treatment your child might have include:
Surgery
Surgery to completely remove the soft tissue sarcoma is done when possible. If the tumor is very large, radiation therapy or chemotherapy may be given first, to make the tumor smaller and decrease the amount of tissue that needs to be removed during surgery. This is called neoadjuvant (preoperative) therapy.
The following types of surgery may be used:
- Wide local excision removes the tumor along with some normal tissue around it.
- Amputation removes all or part of the arm or leg with cancer.
- Lymphadenectomy removes the lymph nodes with cancer.
- Mohs surgery is used to treat cancer in the skin. Individual layers of cancer tissue are removed and checked under a microscope one at a time until all cancer tissue has been removed. This type of surgery is used to treat dermatofibrosarcoma protuberans. It is also called Mohs micrographic surgery.
A second-look surgery may be needed to:
- remove any remaining cancer cells
- check the area around where the tumor was removed for cancer cells and then remove more tissue, if needed
After the doctor removes all the cancer that can be seen at the time of the surgery, some patients may be given chemotherapy or radiation therapy after surgery to kill any cancer cells that are left. Treatment given after the surgery, to lower the risk that the cancer will come back, is called adjuvant therapy.
Learn more about Surgery to Treat Cancer.
Radiation therapy
Radiation therapy is a cancer treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. There are different types of radiation therapy:
- External radiation therapy uses a machine outside the body to send radiation toward the area of the body with cancer. Certain ways of giving radiation therapy can help keep radiation from damaging nearby healthy tissue. This type of radiation therapy may include:
- Stereotactic body radiation therapy uses special equipment to place the patient in the same position for each radiation treatment. Once a day for several days, a radiation machine aims a larger than usual dose of radiation directly at the tumor. By having the patient in the same position for each treatment, there is less damage to nearby healthy tissue. This procedure is also called stereotactic external-beam radiation therapy and stereotaxic radiation therapy.
- Conformal radiation therapy uses a computer to make a 3-dimensional (3-D) picture of the tumor and shapes the radiation beams to fit the tumor. This allows a high dose of radiation to reach the tumor and causes less damage to nearby healthy tissue.
- Intensity-modulated radiation therapy (IMRT) is a type of 3-D radiation therapy that uses a computer to make pictures of the size and shape of the tumor. Thin beams of radiation of different intensities (strengths) are aimed at the tumor from many angles. This type of external radiation therapy causes less damage to nearby healthy tissue.
- Proton beam radiation therapy is a type of high-energy, external radiation therapy that uses streams of protons (tiny particles with a positive charge) to kill tumor cells. This type of treatment can lower the amount of radiation damage to healthy tissue near a tumor.
- Internal radiation therapy uses a radioactive substance sealed in needles, seeds, wires, or catheters that are placed directly into or near the cancer.
The way radiation therapy is given depends on the type and stage of the cancer being treated, if any cancer cells remain after surgery, and the expected side effects of treatment. External and internal radiation therapy are used to treat childhood soft tissue sarcoma.
Learn more about Radiation Therapy to Treat Cancer.
Chemotherapy
Chemotherapy (also called chemo) uses drugs to stop the growth of cancer cells. Chemotherapy either kills the cancer cells or stops them from dividing. Chemotherapy may be given alone or with other types of treatment, such as radiation therapy.
For children with soft tissue sarcoma, chemotherapy is taken by mouth or injected into a vein. When given this way, the drugs enter the bloodstream to reach cancer cells throughout the body.
The way the chemotherapy is given depends on the type of soft tissue sarcoma being treated. Some types of soft tissue sarcoma may respond to treatment with chemotherapy.
Chemotherapy that may be used alone or in combination includes:
Other chemotherapy drugs not listed here may also be used.
Learn more about how chemotherapy works, how it is given, common side effects, and more at Chemotherapy to Treat Cancer.
Observation
Observation is closely monitoring a person's condition without giving any treatment until signs or symptoms appear or change. Observation may be done when:
- complete removal of the tumor is not possible
- no other treatments are available
- the tumor is not likely to damage any vital organs
Observation may be used for epithelioid hemangioendothelioma, infantile fibrosarcoma, or PEComa.
Targeted therapy
Targeted therapy uses drugs or other substances to block the action of specific enzymes, proteins, and other molecules involved in the growth and spread of cancer cells. Targeted therapies used to treat soft tissue sarcoma include:
- Atezolizumab is used to treat children older than 2 years with alveolar soft part sarcoma that can't be removed with surgery or has spread to other places in the body.
- Larotrectinib is used to treat infantile fibrosarcoma.
- Sirolimus may be used to treat PEComas.
- Tazemetostat is used to treat epithelioid sarcoma.
Learn more about Targeted Therapy to Treat Cancer.
Immunotherapy
Immunotherapy is a treatment that uses the person's immune system to fight cancer. Pembrolizumab may be used to treat undifferentiated pleomorphic sarcoma (malignant fibrous histiocytoma) and progressive and recurrent soft tissue sarcoma.
Learn more about Immunotherapy to Treat Cancer.
Clinical trials
For some children, joining a clinical trial may be an option. There are different types of clinical trials for childhood cancer. For example, a treatment trial tests new treatments or new ways of using current treatments. Supportive care and palliative care trials look at ways to improve quality of life, especially for those who have side effects from cancer and its treatment.
You can use the clinical trial search to find NCI-supported cancer clinical trials accepting participants. The search allows you to filter trials based on the type of cancer, your child's age, and where the trials are being done. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Learn more about clinical trials, including how to find and join one, at Clinical Trials Information for Patients and Caregivers.
Treatment of childhood soft tissue sarcoma
To learn about the treatments listed below, visit Types of treatment for childhood soft tissue sarcoma.
Blood vessel tumors
Epithelioid hemangioendothelioma
Treatment of newly diagnosed epithelioid hemangioendothelioma may include:
- surgery to remove the tumor, when possible
- immunotherapy (interferon) for tumors that are likely to spread
- targeted therapy (pazopanib or sirolimus) for tumors that are likely to spread
- chemotherapy
- radiation therapy
- palliative care
Angiosarcoma
Treatment of newly diagnosed angiosarcoma may include:
- surgery to completely remove the tumor
- a combination of surgery, chemotherapy, and radiation therapy for angiosarcomas that have spread
- palliative care
Bone tumors
Extraskeletal osteosarcoma
Treatment of newly diagnosed extraskeletal osteosarcoma is surgery to completely remove the tumor, followed by chemotherapy.
Learn more at Osteosarcoma Treatment.
Cartilage tumors
Extraskeletal mesenchymal chondrosarcoma
Treatment of newly diagnosed extraskeletal mesenchymal chondrosarcoma may include:
- Surgery to completely remove the tumor. Radiation therapy may be given before and/or after surgery.
- Chemotherapy, followed by surgery. Chemotherapy with or without radiation therapy is given after surgery.
Fat tissue tumors
Liposarcoma
Treatment of newly diagnosed liposarcoma may include:
- Surgery to completely remove the tumor. If the cancer is not completely removed, a second surgery may be done.
- Chemotherapy to shrink the tumor, followed by surgery.
- Radiation therapy before or after surgery.
Fibrous connective tissue tumors
Dermatofibrosarcoma protuberans
Treatment of newly diagnosed dermatofibrosarcoma protuberans may include:
- Surgery to completely remove the tumor, when possible. This may include Mohs surgery.
- Radiation therapy before or after surgery.
Fibrosarcoma
Infantile fibrosarcoma
Treatment of newly diagnosed infantile fibrosarcoma may include:
- targeted therapy (larotrectinib)
- surgery to remove the tumor before or after targeted therapy
- chemotherapy before or after surgery and targeted therapy
Adult-type fibrosarcoma
Treatment of adult-type newly diagnosed fibrosarcoma is surgery to completely remove the tumor, when possible.
Myxofibrosarcoma
Treatment of newly diagnosed myxofibrosarcoma is surgery to completely remove the tumor.
Low-grade fibromyxoid sarcoma
Treatment of newly diagnosed low-grade fibromyxoid sarcoma is surgery to completely remove the tumor.
Pericytic (perivascular) tumors
Infantile hemangiopericytoma
Treatment of newly diagnosed infantile hemangiopericytoma is usually chemotherapy.
Skeletal muscle tumors
Rhabdomyosarcoma
Learn more at Childhood Rhabdomyosarcoma Treatment.
Ectomesenchymoma
Treatment of newly diagnosed ectomesenchymoma may include:
- surgery
- chemotherapy
- radiation therapy
So-called fibrohistiocytic tumors
Plexiform fibrohistiocytic tumor
Treatment of newly diagnosed plexiform fibrohistiocytic tumor is surgery to completely remove the tumor.
Tumors of unknown cell origin (the place where the tumor first formed is not known)
Myxoma (Carney complex)
Other summaries with information related to Carney complex include:
Epithelioid sarcoma
Treatment of newly diagnosed epithelioid sarcoma may include:
- surgery to remove the tumor, when possible
- chemotherapy
- radiation therapy before or after surgery
- targeted therapy (tazemetostat)
Extraskeletal myxoid chondrosarcoma
Treatment of newly diagnosed extraskeletal myxoid chondrosarcoma may include:
- surgery to remove the tumor, when possible
- radiation therapy
Extraskeletal Ewing sarcoma
Learn more at Ewing Sarcoma Treatment.
Perivascular epithelioid cell tumors (PEComas)
Treatment of newly diagnosed perivascular epithelioid cell tumors may include:
Undifferentiated or unclassified sarcoma
Undifferentiated pleomorphic sarcoma (malignant fibrous histiocytoma)
Treatment of newly diagnosed undifferentiated pleomorphic sarcoma may include surgery. Treatment of recurrent or refractory undifferentiated pleomorphic sarcoma may include immunotherapy (pembrolizumab).
Learn more about the treatment of malignant fibrous histiocytoma of bone at Osteosarcoma Treatment.
Metastatic childhood soft tissue sarcoma
Treatment of childhood soft tissue sarcoma that has spread to other parts of the body at diagnosis is chemotherapy and radiation therapy. Surgery may be done to remove tumors that have spread to the lung.
To learn more about the treatment of specific tumor types, visit Treatment of Childhood Soft Tissue Sarcoma.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of progressive or recurrent childhood soft tissue sarcoma
To learn about the treatments listed below, visit Types of treatment for childhood soft tissue sarcoma.
Treatment of progressive or recurrent childhood soft tissue sarcoma may include:
- surgery to remove cancer that has come back where it first formed or that has spread to the lungs
- surgery followed by external or internal radiation therapy, if radiation therapy has not already been given
- chemotherapy
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Side effects and late effects of treatment
Cancer treatments can cause side effects. Which side effects your child might have depends on the type of treatment they receive, the dose, and how their body reacts. Talk with your child's treatment team about which side effects to look for and ways to manage them.
To learn more about side effects that begin during treatment for cancer, visit Side Effects.
Problems from cancer treatment that begin 6 months or later after treatment and continue for months or years are called late effects. Late effects of cancer treatment may include:
- physical problems
- changes in mood, feelings, thinking, learning, or memory
- second cancers (new types of cancer)
Some late effects may be treated or controlled. It is important to talk with your child's doctors about the effects cancer treatment can have on your child. Learn more about Late Effects of Treatment for Childhood Cancer.
Prognostic factors for childhood soft tissue sarcoma
If your child has been diagnosed with a soft tissue sarcoma, you may have questions about how serious the cancer is and your child's chances of survival. The likely outcome or course of a disease is called prognosis. The prognosis depends on:
- the part of the body where the tumor first formed
- the size and grade of the tumor
- the type of soft tissue sarcoma
- how deep the tumor is under the skin
- whether the tumor has spread to other places in the body and where it has spread
- the amount of tumor remaining after surgery to remove it
- whether radiation therapy was used to treat the tumor
- whether the cancer has just been diagnosed or has recurred (come back)
No two people are alike, and responses to treatment can vary greatly. Your child's cancer care team is in the best position to talk with you about your child's prognosis.
Follow-up care
As your child goes through treatment, they will have follow-up tests or check-ups. Some of the tests that were done to diagnose the cancer may be repeated to see how well the treatment is working. Decisions about whether to continue, change, or stop treatment may be based on the results of these tests.
Some of the tests will continue to be done from time to time after treatment has ended. The results of these tests can show if your child's condition has changed or if the cancer has recurred (come back).
Learn more about the follow-up tests in Tests to diagnose childhood soft tissue sarcoma.
Coping with your child's cancer
When your child has cancer, every member of the family needs support. Taking care of yourself during this difficult time is important. Reach out to your child's treatment team and to people in your family and community for support. To learn more, visit Support for Families: Childhood Cancer and the booklet Children with Cancer: A Guide for Parents.
Related resources
For more childhood cancer information and other general cancer resources, visit:
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute's (NCI's) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government’s center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about the treatment of childhood soft tissue sarcoma. It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary ("Updated") is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Pediatric Treatment Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become "standard." Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI's website. For more information, call the Cancer Information Service (CIS), NCI's contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as “NCI’s PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary].”
The best way to cite this PDQ summary is:
PDQ® Pediatric Treatment Editorial Board. PDQ Childhood Soft Tissue Sarcoma. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/soft-tissue-sarcoma/patient/child-soft-tissue-treatment-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389342]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website’s E-mail Us.