Male Breast Cancer Treatment (PDQ®)–Patient Version
General Information about Male Breast Cancer
Key Points
- Male breast cancer is a disease in which malignant (cancer) cells form in the tissues of the breast.
- A family history of breast cancer and other factors can increase a man's risk of breast cancer.
- Male breast cancer is sometimes caused by inherited gene mutations (changes).
- Men with breast cancer usually have lumps that can be felt.
- Tests that examine the breasts are used to diagnose breast cancer in men.
- If cancer is found, tests are done to study the cancer cells.
- Survival for men with breast cancer is similar to survival for women with breast cancer.
- Certain factors affect prognosis (chance of recovery) and treatment options.
Male breast cancer is a disease in which malignant (cancer) cells form in the tissues of the breast.
Breast cancer may occur in men. Breast cancer may occur in men at any age, but it usually occurs in men between 60 and 70 years of age. Male breast cancer makes up less than 1% of all cases of breast cancer.
The following types of breast cancer are found in men:
- Infiltrating ductal carcinoma: Cancer that has spread beyond the cells lining ducts in the breast. This is the most common type of breast cancer in men.
- Ductal carcinoma in situ: Abnormal cells that are found in the lining of a duct; also called intraductal carcinoma.
- Inflammatory breast cancer: A type of cancer in which the breast looks red and swollen and feels warm.
- Paget disease of the nipple: A tumor that has grown from ducts beneath the nipple onto the surface of the nipple.
Lobular carcinoma in situ (abnormal cells found in one of the lobes or sections of the breast), which sometimes occurs in women, has not been seen in men.
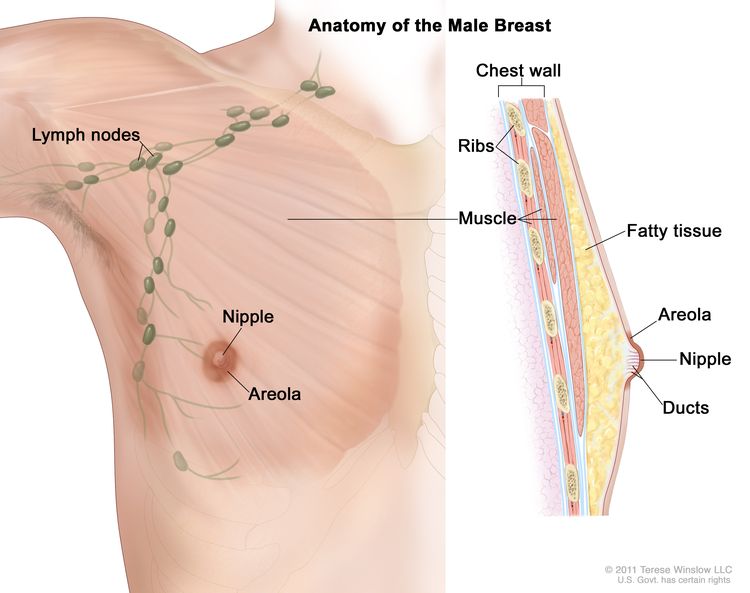
A family history of breast cancer and other factors can increase a man's risk of breast cancer.
Anything that increases your risk of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesn’t mean that you will not get cancer. Talk with your doctor if you think you may be at risk. Risk factors for breast cancer in men may include the following:
- Treatment with radiation therapy to your breast/chest.
- Having a disease linked to high levels of estrogen in the body, such as cirrhosis (liver disease) or Klinefelter syndrome (a genetic disorder).
- Having one or more female relatives who have had breast cancer.
- Having mutations (changes) in genes such as BRCA2.
Male breast cancer is sometimes caused by inherited gene mutations (changes).
The genes in cells carry the hereditary information that is received from a person's parents. Hereditary breast cancer makes up about 5% to 10% of all breast cancer. Some mutated genes related to breast cancer, such as BRCA2, are more common in certain ethnic groups. Men who have a mutated gene related to breast cancer have an increased risk of this disease.
There are tests that can detect (find) mutated genes. These genetic tests are sometimes done for members of families with a high risk of cancer. See the following PDQ summaries for more information:
Men with breast cancer usually have lumps that can be felt.
Lumps and other signs may be caused by male breast cancer or by other conditions. Check with your doctor if you have any of the following:
- A lump or thickening in or near the breast or in the underarm area.
- A change in the size or shape of the breast.
- A dimple or puckering in the skin of the breast.
- A nipple turned inward into the breast.
- Fluid from the nipple, especially if it's bloody.
- Scaly, red, or swollen skin on the breast, nipple, or areola (the dark area of skin around the nipple).
- Dimples in the breast that look like the skin of an orange, called peau d’orange.
Tests that examine the breasts are used to diagnose breast cancer in men.
The following tests and procedures may be used:
- Physical exam and health history: An exam of the body to check general signs of health, including checking for signs of disease, such as lumps or anything else that seems unusual. A history of the patient’s health habits and past illnesses and treatments will also be taken.
- Clinical breast exam (CBE): An exam of the breast by a doctor or other health professional. The doctor will carefully feel the breasts and under the arms for lumps or anything else that seems unusual.
- Mammogram: An x-ray of the breast.
- Ultrasound exam: A procedure in which high-energy sound waves (ultrasound) are bounced off internal tissues or organs and make echoes. The echoes form a picture of body tissues called a sonogram. The picture can be printed to be looked at later.
- MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of both breasts. This procedure is also called nuclear magnetic resonance imaging (NMRI).
- Blood chemistry studies: A procedure in which a blood sample is checked to measure the amounts of certain substances released into the blood by organs and tissues in the body. An unusual (higher or lower than normal) amount of a substance can be a sign of disease.
- Biopsy: The removal of cells or tissues so they can be viewed under a microscope by a pathologist to check for signs of cancer. There are four types of biopsies to check for breast cancer:
- Excisional biopsy: The removal of an entire lump of tissue.
- Incisional biopsy: The removal of part of a lump or a sample of tissue.
- Core biopsy: The removal of tissue using a wide needle.
- Fine-needle aspiration (FNA) biopsy: The removal of tissue or fluid using a thin needle.
If cancer is found, tests are done to study the cancer cells.
Decisions about the best treatment are based on the results of these tests. The tests give information about:
- How quickly the cancer may grow.
- How likely it is that the cancer will spread through the body.
- How well certain treatments might work.
- How likely the cancer is to recur (come back).
Tests include the following:
- Estrogen and progesterone receptor test: A test to measure the amount of estrogen and progesterone (hormones) receptors in cancer tissue. If there are more estrogen and progesterone receptors than normal, the cancer is called estrogen and/or progesterone receptor positive. This type of breast cancer may grow more quickly. The test results show whether treatment to block estrogen and progesterone may stop the cancer from growing.
- HER2 test: A laboratory test to measure how many HER2/neu genes there are and how much HER2/neu protein is made in a sample of tissue. If there are more HER2/neu genes or higher levels of HER2/neu protein than normal, the cancer is called HER2/neu positive. This type of breast cancer may grow more quickly and is more likely to spread to other parts of the body. The cancer may be treated with drugs that target the HER2/neu protein, such as trastuzumab and pertuzumab.
Survival for men with breast cancer is similar to survival for women with breast cancer.
Survival for men with breast cancer is similar to that for women with breast cancer when their stage at diagnosis is the same. Breast cancer in men, however, is often diagnosed at a later stage. Cancer found at a later stage may be less likely to be cured.
Certain factors affect prognosis (chance of recovery) and treatment options.
The prognosis and treatment options depend on the following:
- The stage of the cancer (the size of the tumor and whether it is in the breast only or has spread to lymph nodes or other places in the body).
- The type of breast cancer.
- Estrogen-receptor and progesterone-receptor levels in the tumor tissue.
- Whether the cancer is also found in the other breast.
- The man's age and general health.
- Whether the cancer has just been diagnosed or has recurred (come back).
Stages of Male Breast Cancer
Key Points
- After breast cancer has been diagnosed, tests are done to find out if cancer cells have spread within the breast or to other parts of the body.
- There are three ways that cancer spreads in the body.
- Cancer may spread from where it began to other parts of the body.
- In breast cancer, stage is based on the size and location of the primary tumor, the spread of cancer to nearby lymph nodes or other parts of the body, tumor grade, and whether certain biomarkers are present.
- The TNM system is used to describe the size of the primary tumor and the spread of cancer to nearby lymph nodes or other parts of the body.
- Tumor (T). The size and location of the tumor.
- Lymph Node (N). The size and location of lymph nodes where cancer has spread.
- Metastasis (M). The spread of cancer to other parts of the body.
- The grading system is used to describe how quickly a breast tumor is likely to grow and spread.
- Biomarker testing is used to find out whether breast cancer cells have certain receptors.
- The TNM system, the grading system, and biomarker status are combined to find out the breast cancer stage.
- Talk to your doctor to find out what your breast cancer stage is and how it is used to plan the best treatment for you.
- The treatment of male breast cancer depends partly on the stage of the disease.
After breast cancer has been diagnosed, tests are done to find out if cancer cells have spread within the breast or to other parts of the body.
After breast cancer has been diagnosed, tests are done to find out if cancer cells have spread within the breast or to other parts of the body. This process is called staging. The information gathered from the staging process determines the stage of the disease. It is important to know the stage in order to plan treatment. Breast cancer in men is staged the same as it is in women. The spread of cancer from the breast to lymph nodes and other parts of the body appears to be similar in men and women.
The following tests and procedures may be used in the staging process:
- Sentinel lymph node biopsy: The removal of the sentinel lymph node during surgery. The sentinel lymph node is the first lymph node in a group of lymph nodes to receive lymphatic drainage from the primary tumor. It is the first lymph node the cancer is likely to spread to from the primary tumor. A radioactive substance and/or blue dye is injected near the tumor. The substance or dye flows through the lymph ducts to the lymph nodes. The first lymph node to receive the substance or dye is removed. A pathologist views the tissue under a microscope to look for cancer cells. If cancer cells are not found, it may not be necessary to remove more lymph nodes. Sometimes, a sentinel lymph node is found in more than one group of nodes.
- Chest x-ray: An x-ray of the organs and bones inside the chest. An x-ray is a type of energy beam that can go through the body and onto film, making a picture of areas inside the body.
- CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside the body, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
- Bone scan: A procedure to check if there are rapidly dividing cells, such as cancer cells, in the bone. A very small amount of radioactive material is injected into a vein and travels through the bloodstream. The radioactive material collects in the bones with cancer and is detected by a scanner.
- PET scan (positron emission tomography scan): A procedure to find malignant tumor cells in the body. A small amount of radioactive glucose (sugar) is injected into a vein. The PET scanner rotates around the body and makes a picture of where glucose is being used in the body. Malignant tumor cells show up brighter in the picture because they are more active and take up more glucose than normal cells do.
There are three ways that cancer spreads in the body.
Cancer can spread through tissue, the lymph system, and the blood:
- Tissue. The cancer spreads from where it began by growing into nearby areas.
- Lymph system. The cancer spreads from where it began by getting into the lymph system. The cancer travels through the lymph vessels to other parts of the body.
- Blood. The cancer spreads from where it began by getting into the blood. The cancer travels through the blood vessels to other parts of the body.
Cancer may spread from where it began to other parts of the body.
When cancer spreads to another part of the body, it is called metastasis. Cancer cells break away from where they began (the primary tumor) and travel through the lymph system or blood.
- Lymph system. The cancer gets into the lymph system, travels through the lymph vessels, and forms a tumor (metastatic tumor) in another part of the body.
- Blood. The cancer gets into the blood, travels through the blood vessels, and forms a tumor (metastatic tumor) in another part of the body.
The metastatic tumor is the same type of cancer as the primary tumor. For example, if breast cancer spreads to the bone, the cancer cells in the bone are actually breast cancer cells. The disease is metastatic breast cancer, not bone cancer.
In breast cancer, stage is based on the size and location of the primary tumor, the spread of cancer to nearby lymph nodes or other parts of the body, tumor grade, and whether certain biomarkers are present.
To plan the best treatment and understand your prognosis, it is important to know the breast cancer stage.
There are 3 types of breast cancer stage groups:
- Clinical Prognostic Stage is used first to assign a stage for all patients based on health history, physical exam, imaging tests (if done), and biopsies. The Clinical Prognostic Stage is described by the TNM system, tumor grade, and biomarker status (ER, PR, HER2). In clinical staging, mammography or ultrasound is used to check the lymph nodes for signs of cancer.
- Pathological Prognostic Stage is then used for patients who have surgery as their first treatment. The Pathological Prognostic Stage is based on all clinical information, biomarker status, and laboratory test results from breast tissue and lymph nodes removed during surgery.
- Anatomic Stage is based on the size and the spread of cancer as described by the TNM system. The Anatomic Stage is used in parts of the world where biomarker testing is not available. It is not used in the United States.
The TNM system is used to describe the size of the primary tumor and the spread of cancer to nearby lymph nodes or other parts of the body.
For breast cancer, the TNM system describes the tumor as follows:
Tumor (T). The size and location of the tumor.
- TX: Primary tumor cannot be assessed.
- T0: No sign of a primary tumor in the breast.
- Tis: Carcinoma in situ. There are 2 types of breast carcinoma in situ:
- Tis (DCIS): DCIS is a condition in which abnormal cells are found in the lining of a breast duct. The abnormal cells have not spread outside the duct to other tissues in the breast. In some cases, DCIS may become invasive breast cancer that is able to spread to other tissues. At this time, there is no way to know which lesions can become invasive.
- Tis (Paget disease): Paget disease of the nipple is a condition in which abnormal cells are found in the skin cells of the nipple and may spread to the areola. It is not staged according to the TNM system. If Paget disease AND an invasive breast cancer are present, the TNM system is used to stage the invasive breast cancer.
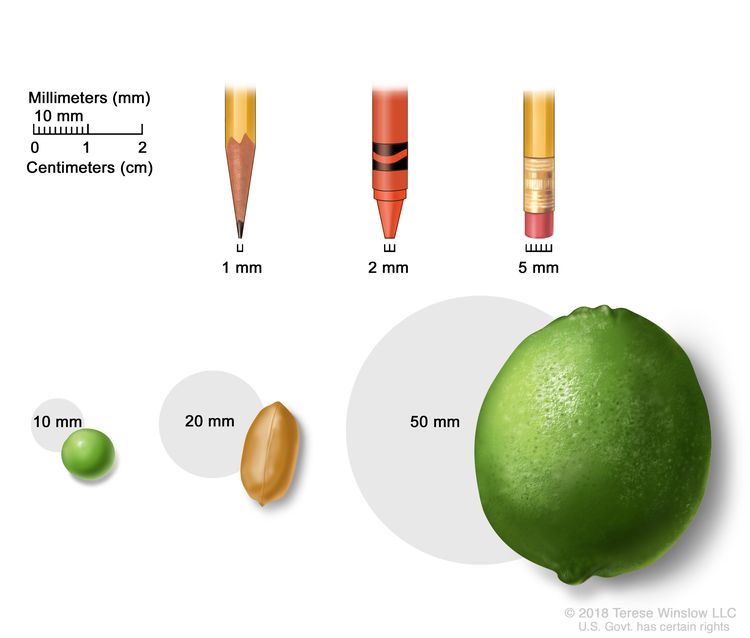
- T1: The tumor is 20 millimeters or smaller. There are 4 subtypes of a T1 tumor depending on the size of the tumor:
- T1mi: the tumor is 1 millimeter or smaller.
- T1a: the tumor is larger than 1 millimeter but not larger than 5 millimeters.
- T1b: the tumor is larger than 5 millimeters but not larger than 10 millimeters.
- T1c: the tumor is larger than 10 millimeters but not larger than 20 millimeters.
- T2: The tumor is larger than 20 millimeters but not larger than 50 millimeters.
- T3: The tumor is larger than 50 millimeters.
- T4: The tumor is described as one of the following:
- T4a: the tumor has grown into the chest wall.
- T4b: the tumor has grown into the skin—an ulcer has formed on the surface of the skin on the breast, small tumor nodules have formed in the same breast as the primary tumor, and/or there is swelling of the skin on the breast.
- T4c: the tumor has grown into the chest wall and the skin.
- T4d: inflammatory breast cancer—one-third or more of the skin on the breast is red and swollen (called peau d'orange).
Lymph Node (N). The size and location of lymph nodes where cancer has spread.
When the lymph nodes are removed by surgery and studied under a microscope by a pathologist, pathologic staging is used to describe the lymph nodes. The pathologic staging of lymph nodes is described below.
- NX: The lymph nodes cannot be assessed.
- N0: No sign of cancer in the lymph nodes, or tiny clusters of cancer cells not larger than 0.2 millimeters in the lymph nodes.
- N1: Cancer is described as one of the following:
- N1mi: cancer has spread to the axillary (armpit area) lymph nodes and is larger than 0.2 millimeters but not larger than 2 millimeters.
- N1a: cancer has spread to 1 to 3 axillary lymph nodes and the cancer in at least one of the lymph nodes is larger than 2 millimeters.
- N1b: cancer has spread to lymph nodes near the breastbone on the same side of the body as the primary tumor, and the cancer is larger than 0.2 millimeters and is found by sentinel lymph node biopsy. Cancer is not found in the axillary lymph nodes.
- N1c: cancer has spread to 1 to 3 axillary lymph nodes and the cancer in at least one of the lymph nodes is larger than 2 millimeters. Cancer is also found by sentinel lymph node biopsy in the lymph nodes near the breastbone on the same side of the body as the primary tumor.
- N2: Cancer is described as one of the following:
- N2a: cancer has spread to 4 to 9 axillary lymph nodes and the cancer in at least one of the lymph nodes is larger than 2 millimeters.
- N2b: cancer has spread to lymph nodes near the breastbone and the cancer is found by imaging tests. Cancer is not found in the axillary lymph nodes by sentinel lymph node biopsy or lymph node dissection.
- N3: Cancer is described as one of the following:
- N3a: cancer has spread to 10 or more axillary lymph nodes and the cancer in at least one of the lymph nodes is larger than 2 millimeters, or cancer has spread to lymph nodes below the collarbone.
- N3b: cancer has spread to 1 to 9 axillary lymph nodes and the cancer in at least one of the lymph nodes is larger than 2 millimeters. Cancer has also spread to lymph nodes near the breastbone and the cancer is found by imaging tests;
or
cancer has spread to 4 to 9 axillary lymph nodes and cancer in at least one of the lymph nodes is larger than 2 millimeters. Cancer has also spread to lymph nodes near the breastbone on the same side of the body as the primary tumor, and the cancer is larger than 0.2 millimeters and is found by sentinel lymph node biopsy.
- N3c: cancer has spread to lymph nodes above the collarbone on the same side of the body as the primary tumor.
When the lymph nodes are checked using mammography or ultrasound, it is called clinical staging. The clinical staging of lymph nodes is not described here.
Metastasis (M). The spread of cancer to other parts of the body.
- M0: There is no sign that cancer has spread to other parts of the body.
- M1: Cancer has spread to other parts of the body, most often the bones, lungs, liver, or brain. If cancer has spread to distant lymph nodes, the cancer in the lymph nodes is larger than 0.2 millimeters. The cancer is called metastatic breast cancer.
The grading system is used to describe how quickly a breast tumor is likely to grow and spread.
The grading system describes a tumor based on how abnormal the cancer cells and tissue look under a microscope and how quickly the cancer cells are likely to grow and spread. Low-grade cancer cells look more like normal cells and tend to grow and spread more slowly than high-grade cancer cells. To describe how abnormal the cancer cells and tissue are, the pathologist will assess the following three features:
- How much of the tumor tissue has normal breast ducts.
- The size and shape of the nuclei in the tumor cells.
- How many dividing cells are present, which is a measure of how fast the tumor cells are growing and dividing.
For each feature, the pathologist assigns a score of 1 to 3; a score of “1” means the cells and tumor tissue look the most like normal cells and tissue, and a score of “3” means the cells and tissue look the most abnormal. The scores for each feature are added together to get a total score between 3 and 9.
Three grades are possible:
- Total score of 3 to 5: G1 (Low grade or well differentiated).
- Total score of 6 to 7: G2 (Intermediate grade or moderately differentiated).
- Total score of 8 to 9: G3 (High grade or poorly differentiated).
Biomarker testing is used to find out whether breast cancer cells have certain receptors.
Healthy breast cells, and some breast cancer cells, have receptors (biomarkers) that attach to the hormones estrogen and progesterone. These hormones are needed for healthy cells, and some breast cancer cells, to grow and divide. To check for these biomarkers, samples of tissue containing breast cancer cells are removed during a biopsy or surgery. The samples are tested in a laboratory to see whether the breast cancer cells have estrogen or progesterone receptors.
Another type of receptor (biomarker) that is found on the surface of all breast cancer cells is called HER2. HER2 receptors are needed for the breast cancer cells to grow and divide.
For breast cancer, biomarker testing includes the following:
- Estrogen receptor (ER). If the breast cancer cells have estrogen receptors, the cancer cells are called ER positive (ER+). If the breast cancer cells do not have estrogen receptors, the cancer cells are called ER negative (ER-).
- Progesterone receptor (PR). If the breast cancer cells have progesterone receptors, the cancer cells are called PR positive (PR+). If the breast cancer cells do not have progesterone receptors, the cancer cells are called PR negative (PR-).
- Human epidermal growth factor type 2 receptor (HER2/neu or HER2). If the breast cancer cells have larger than normal amounts of HER2 receptors on their surface, the cancer cells are called HER2 positive (HER2+). If the breast cancer cells have a normal amount of HER2 on their surface, the cancer cells are called HER2 negative (HER2-). HER2+ breast cancer is more likely to grow and divide faster than HER2- breast cancer.
Sometimes the breast cancer cells will be described as triple negative or triple positive.
- Triple negative. If the breast cancer cells do not have estrogen receptors, progesterone receptors, or a larger than normal amount of HER2 receptors, the cancer cells are called triple negative.
- Triple positive. If the breast cancer cells do have estrogen receptors, progesterone receptors, and a larger than normal amount of HER2 receptors, the cancer cells are called triple positive.
It is important to know the estrogen receptor, progesterone receptor, and HER2 receptor status to choose the best treatment. There are drugs that can stop the receptors from attaching to the hormones estrogen and progesterone and stop the cancer from growing. Other drugs may be used to block the HER2 receptors on the surface of the breast cancer cells and stop the cancer from growing.
The TNM system, the grading system, and biomarker status are combined to find out the breast cancer stage.
Here are 3 examples that combine the TNM system, the grading system, and the biomarker status to find out the Pathological Prognostic breast cancer stage for a woman whose first treatment was surgery:
If the tumor size is 30 millimeters (T2), has not spread to nearby lymph nodes (N0), has not spread to distant parts of the body (M0), and is:
- Grade 1
- HER2+
- ER-
- PR-
The cancer is stage IIA.
If the tumor size is 53 millimeters (T3), has spread to 4 to 9 axillary lymph nodes (N2), has not spread to other parts of the body (M0), and is:
- Grade 2
- HER2+
- ER+
- PR-
The tumor is stage IIIA.
If the tumor size is 65 millimeters (T3), has spread to 3 axillary lymph nodes (N1a), has spread to the lungs (M1), and is:
- Grade 1
- HER2+
- ER-
- PR-
The cancer is stage IV (metastatic breast cancer).
Talk to your doctor to find out what your breast cancer stage is and how it is used to plan the best treatment for you.
After surgery, your doctor will receive a pathology report that describes the size and location of the primary tumor, the spread of cancer to nearby lymph nodes, tumor grade, and whether certain biomarkers are present. The pathology report and other test results are used to determine your breast cancer stage.
You are likely to have many questions. Ask your doctor to explain how staging is used to decide the best options to treat your cancer and whether there are clinical trials that might be right for you.
The treatment of male breast cancer depends partly on the stage of the disease.
For treatment options for stage I, stage II, stage IIIA, and operable stage IIIC breast cancer, see Treatment of Early/Localized/Operable Male Breast Cancer.
For treatment options for cancer that has recurred (come back) near the area where it first formed, see Treatment of Locoregional Recurrent Male Breast Cancer.
For treatment options for stage IV (metastatic) breast cancer or breast cancer that has recurred in other parts of the body, see Treatment of Metastatic Male Breast Cancer.
Inflammatory Male Breast Cancer
In inflammatory breast cancer, cancer has spread to the skin of the breast and the breast looks red and swollen and feels warm. The redness and warmth occur because the cancer cells block the lymph vessels in the skin. The skin of the breast may also show the dimpled appearance called peau d’orange (like the skin of an orange). There may not be any lumps in the breast that can be felt. Inflammatory breast cancer may be stage IIIB, stage IIIC, or stage IV.
Treatment Option Overview
Key Points
- There are different types of treatment for men with breast cancer.
- Five types of standard treatment are used to treat men with
breast cancer:
- Surgery
- Chemotherapy
- Hormone therapy
- Radiation therapy
- Targeted therapy
- Treatment for male breast cancer may cause side effects.
There are different types of treatment for men with breast cancer.
Different types of treatment are available for men with breast cancer. Some treatments are standard (the currently used treatment), and some are being tested in clinical trials. A treatment clinical trial is a research study meant to help improve current treatments or obtain information on new treatments for patients with cancer. When clinical trials show that a new treatment is better than the standard treatment, the new treatment may become the standard treatment.
For some patients, taking part in a clinical trial may be the best treatment choice. Many of today's standard treatments for cancer are based on earlier clinical trials. Patients who take part in a clinical trial may receive the standard treatment or be among the first to receive a new treatment.
Patients who take part in clinical trials also help improve the way cancer will be treated in the future. Even when clinical trials do not lead to effective new treatments, they often answer important questions and help move research forward.
Some clinical trials only include patients who have not yet received treatment. Other trials test treatments for patients whose cancer has not gotten better. There are also clinical trials that test new ways to stop cancer from recurring (coming back) or reduce the side effects of cancer treatment.
Clinical trials are taking place in many parts of the country. Information about clinical trials is available from the NCI website. Choosing the most appropriate cancer treatment is a decision that ideally involves the patient, family, and health care team.
Five types of standard treatment are used to treat men with breast cancer:
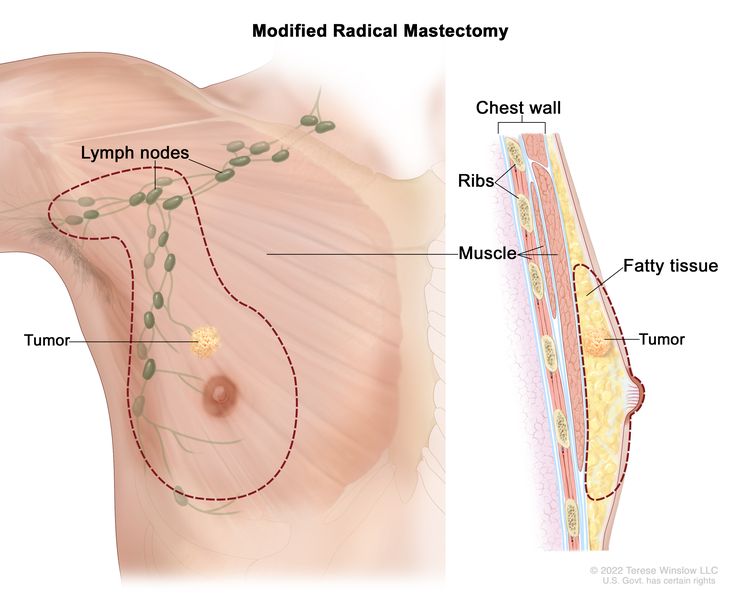
Surgery
Surgery for men with breast cancer is usually a modified radical mastectomy, surgery to remove the whole breast that has cancer. This may include removal of the nipple, areola (the dark-colored skin around the nipple), and skin over the breast. Most of the lymph nodes under the arm are also removed.
Breast-conserving
surgery, an operation to remove the cancer but not the breast
itself, is also used for some men with breast cancer. A lumpectomy is done to remove the tumor (lump) and a small amount of normal tissue around it. Radiation therapy is given after surgery to kill any cancer cells that are left.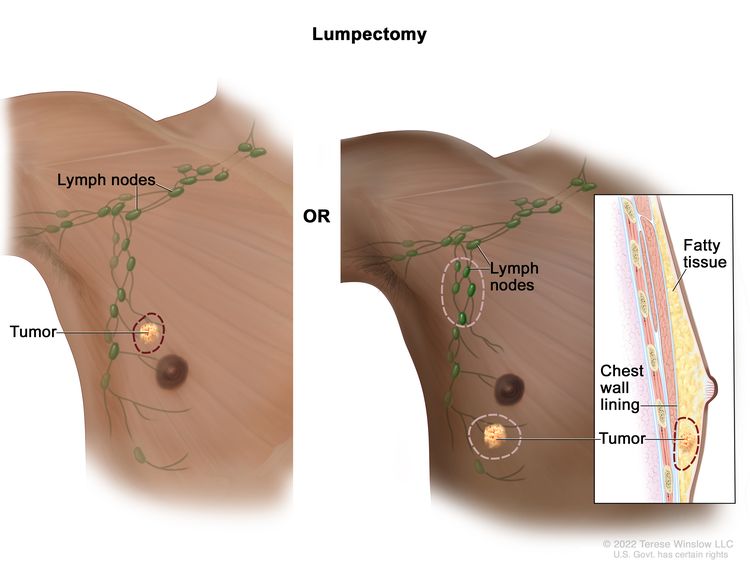
Chemotherapy
Chemotherapy is a cancer treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. When chemotherapy is taken by mouth or injected into a vein or muscle, the drugs enter the bloodstream and can reach cancer cells throughout the body (systemic chemotherapy).
See Drugs Approved for Breast Cancer for more information.
Hormone therapy
Hormone therapy is a cancer treatment that removes hormones or blocks their action and stops cancer cells from growing. Hormones are substances made by glands in the body and circulated in the bloodstream. Some hormones can cause certain cancers to grow. If tests show that the cancer cells have places where hormones can attach (receptors), drugs, surgery, or radiation therapy is used to reduce the production of hormones or block them from working.
Hormone therapy with tamoxifen is often given to patients with estrogen-receptor and progesterone-receptor positive breast cancer and to patients with metastatic breast cancer (cancer that has spread to other parts of the body).
Hormone therapy with an aromatase inhibitor is given to some men who have metastatic breast cancer. Aromatase inhibitors decrease the body's estrogen by blocking an enzyme called aromatase from turning androgen into estrogen. Anastrozole, letrozole, and exemestane are types of aromatase inhibitors.
Hormone therapy with a luteinizing hormone-releasing hormone (LHRH) agonist is given to some men who have metastatic breast cancer. LHRH agonists affect the pituitary gland, which controls how much testosterone is made by the testicles. In men who are taking LHRH agonists, the pituitary gland tells the testicles to make less testosterone. Leuprolide and goserelin are types of LHRH agonists.
Other types of hormone therapy include megestrol acetate or anti-estrogen therapy, such as fulvestrant.
See Drugs Approved for Breast Cancer for more information.
Radiation therapy
Radiation therapy is a cancer treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. External radiation therapy uses a machine outside the body to send radiation toward the area of the body with cancer.
Targeted therapy
Targeted therapy is a type of treatment that uses drugs or other substances to identify and attack specific cancer cells. Targeted therapies usually cause less harm to normal cells than chemotherapy or radiation therapy do. Monoclonal antibody therapy, tyrosine kinase inhibitors, cyclin-dependent kinase inhibitors, and mammalian target of rapamycin (mTOR) inhibitors are types of targeted therapies used to treat men with breast cancer.
Monoclonal antibodies are immune system proteins made in the laboratory to treat many diseases, including cancer. As a cancer treatment, these antibodies can attach to a specific target on cancer cells or other cells that may help cancer cells grow. The antibodies are able to then kill the cancer cells, block their growth, or keep them from spreading. Monoclonal antibodies are given by infusion. They may be used alone or to carry drugs, toxins, or radioactive material directly to cancer cells.
Types of monoclonal antibody therapy include the following:
- Trastuzumab is a monoclonal antibody that blocks the effects of the growth factor protein HER2.
- Pertuzumab is a monoclonal antibody that may be combined with trastuzumab and chemotherapy to treat breast cancer.
- Ado-trastuzumab emtansine is a monoclonal antibody linked to an anticancer drug. This is called an antibody-drug conjugate. It may be used to treat men with hormone receptor positive breast cancer that has spread to other parts of the body.
Tyrosine kinase inhibitors are targeted therapy drugs that block signals needed for tumors to grow. Lapatinib is a tyrosine kinase inhibitor that may be used to treat men with metastatic breast cancer.
Cyclin-dependent kinase inhibitors are targeted therapy drugs that block proteins called cyclin-dependent kinases, which cause the growth of cancer cells. Palbociclib is a cyclin-dependent kinase inhibitor used to treat men with metastatic breast cancer.
Mammalian target of rapamycin (mTOR) inhibitors block a protein called mTOR, which may keep cancer cells from growing and prevent the growth of new blood vessels that tumors need to grow.
See Drugs Approved for Breast Cancer for more information.
Treatment for male breast cancer may cause side effects.
For information about side effects caused by treatment for cancer, visit our Side Effects page.
Treatment of Early/Localized/Operable Male Breast Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of early, localized, or operable breast cancer may include the following:
Initial Surgery
Treatment for men diagnosed with breast cancer is usually modified radical mastectomy.
Breast-conserving surgery with lumpectomy followed by radiation therapy may be used for some men.
Adjuvant Therapy
Therapy given after an operation when cancer cells can no longer be seen is called adjuvant therapy. Even if the doctor removes all the cancer that can be seen at the time of the operation, the patient may be given radiation therapy, chemotherapy, hormone therapy, and/or targeted therapy after surgery, to try to kill any cancer cells that may be left.
- Node-negative: For men whose cancer is node-negative (cancer has not spread to the lymph nodes), adjuvant therapy should be considered on the same basis as for a woman with breast cancer because there is no evidence that response to therapy is different for men and women.
- Node-positive:
For men whose cancer is node-positive (cancer has spread to the lymph nodes),
adjuvant therapy may include the following:
- Chemotherapy.
- Hormone therapy with tamoxifen (to block the effect of estrogen) or less often, aromatase inhibitors (to reduce the amount of estrogen in the body).
- Targeted therapy with a monoclonal antibody (trastuzumab or pertuzumab).
These treatments appear to increase survival in men as they do in women. The patient's response to hormone therapy depends on whether there are hormone receptors (proteins) in the tumor. Most breast cancers in men have these receptors. Hormone therapy is usually recommended for male breast cancer patients, but it can have many side effects, including hot flashes and impotence (the inability to have an erection adequate for sexual intercourse).
Treatment of Locoregional Recurrent Male Breast Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
For men with locally recurrent disease (cancer that has come back in a limited area after treatment), treatment options include:
- Surgery.
- Radiation therapy combined with chemotherapy.
Treatment of Metastatic Male Breast Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment options for metastatic breast cancer (cancer that has spread to distant parts of the body) may include the following:
Hormone therapy
In men who have just been diagnosed with metastatic breast cancer that is hormone receptor positive or if the hormone receptor status is not known, treatment may include:
- Tamoxifen therapy.
- Aromatase inhibitor therapy (anastrozole, letrozole, or exemestane) with or without an LHRH agonist. Sometimes cyclin-dependent kinase inhibitor therapy (palbociclib) is also given.
In men whose tumors are hormone receptor positive or hormone receptor unknown, with spread to the bone or soft tissue only, and who have been treated with tamoxifen, treatment may include:
- Aromatase inhibitor therapy with or without LHRH agonist.
- Other hormone therapy such as megestrol acetate, estrogen or androgen therapy, or anti-estrogen therapy such as fulvestrant.
Targeted therapy
In men with metastatic breast cancer that is hormone receptor positive and has not responded to other treatments, options may include targeted therapy such as:
- Trastuzumab, lapatinib, pertuzumab, or mTOR inhibitors.
- Antibody-drug conjugate therapy with ado-trastuzumab emtansine.
- Cyclin-dependent kinase inhibitor therapy (palbociclib) combined with letrozole.
In men with metastatic breast cancer that is HER2/neu positive, treatment may include:
- Targeted therapy such as trastuzumab, pertuzumab, ado-trastuzumab emtansine, or lapatinib.
Chemotherapy
In men with metastatic breast cancer that is hormone receptor negative, has not responded to hormone therapy, has spread to other organs or has caused symptoms, treatment may include:
- Chemotherapy with one or more drugs.
Surgery
- Total mastectomy for men with open or painful breast lesions. Radiation therapy may be given after surgery.
- Surgery to remove cancer that has spread to the brain or spine. Radiation therapy may be given after surgery.
- Surgery to remove cancer that has spread to the lung.
- Surgery to repair or help support weak or broken bones. Radiation therapy may be given after surgery.
- Surgery to remove fluid that has collected around the lungs or heart.
Radiation therapy
- Radiation therapy to the bones, brain, spinal cord, breast, or chest wall to relieve symptoms and improve quality of life.
- Strontium-89 (a radionuclide) to relieve pain from cancer that has spread to bones throughout the body.
Other treatment options
Other treatment options for metastatic breast cancer include:
- Drug therapy with bisphosphonates or denosumab to reduce bone disease and pain when cancer has spread to the bone. (See the PDQ summary on Cancer Pain for more information about bisphosphonates.)
- Clinical trials testing new anticancer drugs, new drug combinations, and new ways of giving treatment.
To Learn More About Male Breast Cancer
For more information from the National Cancer Institute about male breast cancer, see the following:
For general cancer information and other resources from the National Cancer Institute, visit:
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute's (NCI's) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government’s center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about the treatment of male breast cancer. It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary ("Updated") is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Adult Treatment Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become "standard." Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI's website. For more information, call the Cancer Information Service (CIS), NCI's contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as “NCI’s PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary].”
The best way to cite this PDQ summary is:
PDQ® Adult Treatment Editorial Board. PDQ Male Breast Cancer Treatment. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/breast/patient/male-breast-treatment-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389417]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website’s E-mail Us.